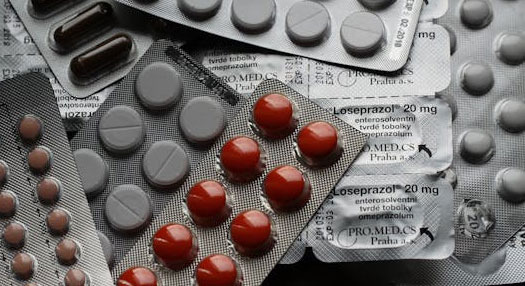
Just because you have health insurance in the U.S. does not mean that all medication costs are covered.
It can be quite shocking when you present a prescription at the pharmacy, only to be told that it is not covered by insurance and you need to pay hundreds of dollars. The U.S. health insurance system is more complicated than expected, with clear criteria distinguishing between covered and non-covered medications.
In the U.S., health insurance typically operates a list of medications known as a 'formulary.'
This is essentially a list of medications that the insurance company covers, and any medications not included on this list are the patient's responsibility. For example, even if two headache medications are the same, the generic version may be covered by insurance, while a brand-name new drug not on the list must be paid for entirely by the patient.
From the insurance company's perspective, reducing costs is the top priority, so they often exclude medications that already have generics or new drugs that are expensive relative to their effectiveness. Therefore, even if a doctor prescribes a medication, it is common for the pharmacist to say, "This is not covered by insurance."
Insurance is fundamentally designed for 'disease treatment purposes.' Therefore, medications that do not pose a direct threat to health, such as those for cosmetic or convenience purposes, are generally not covered. Medications for erectile dysfunction, for example, are classified as not being "medically necessary treatment," even if they are widely used, so the patient is typically responsible for the cost.
Over-the-counter medications like cold medicine, digestive aids, and allergy medications are also not covered by insurance. Even with a doctor's prescription, if the medication is classified as OTC, it must be purchased directly at the pharmacy. For instance, allergy medication Claritin is not covered by insurance, even if prescribed by a doctor, and must be purchased directly from the pharmacy shelf.
When a new drug is released in the U.S., it must receive FDA approval, and afterward, insurance companies decide whether to cover it. However, newly released drugs are often not covered immediately due to reasons like "insufficient data" or "too expensive." Especially for medications for rare diseases that can cost thousands to tens of thousands of dollars, patients often need to seek support through manufacturer programs.
Additionally, medications provided during clinical trials are not covered by insurance. These are usually provided free of charge to clinical trial participants by the pharmaceutical company. Some medications have approved uses, but doctors may prescribe them for different purposes. This is referred to as 'off-label use,' and in such cases, insurance companies may deny coverage on the grounds of "unapproved use." For example, using antidepressants for treating insomnia is a common case. Even if it may be effective, it is not covered under insurance regulations.
Furthermore, vitamins, minerals, and dietary supplements are not covered by insurance. Even if recommended by a doctor, they must be purchased directly at the pharmacy. However, there are exceptional cases where coverage is provided for patients with specific conditions (e.g., special vitamins needed for dialysis patients), but this is not common.
Dental and Vision Medications
One of the major characteristics of U.S. insurance is that dental and vision care are not included in basic health insurance. Separate insurance is required for coverage, and otherwise, all related medications are the patient's responsibility. Antibiotics needed for cavity treatment and eye drops for dry eyes are often excluded from general health insurance.
Some Mental Health Medications
Not all psychiatric medications are covered. Commonly used antidepressants and anti-anxiety medications are covered, but new drugs or specific brand-name medications may be excluded. Insurance companies encourage the use of generics whenever possible, and if a brand-name medication is desired, the doctor often needs to submit a separate document for 'Medical Necessity.'
U.S. health insurance is not a concept of "covering all medication costs." Coverage varies based on the formulary (medication list) operated by each insurance company, and most costs for cosmetic and convenience purposes, OTC medications, new drugs, off-label use, and vitamins are the patient's responsibility.
Therefore, having health insurance in the U.S. should not provide a false sense of security; when prescribed a new medication, it is essential to first check with the pharmacy, "Is this covered by insurance?"
In some cases, the insurance company may designate alternative medications, and pharmaceutical companies may operate patient support programs, so with a little research, there may be ways to reduce the financial burden.








 Gouch Caps |
Gouch Caps | 
 Who's watching? |
Who's watching? | 
 Pinky Seven |
Pinky Seven | 
 river9 |
river9 | 
 RV Samuel's Dad |
RV Samuel's Dad | 
 U.S. College Admission Information |
U.S. College Admission Information | 
 Samttugi Grasshopper Noodle |
Samttugi Grasshopper Noodle | 
 US Home Buying Information Home Insurance |
US Home Buying Information Home Insurance | 
 The Day the Sun Rises |
The Day the Sun Rises |